At Orthopaedic Institute of Ohio, our goal is to treat your aches and pains and get you back to enjoying your favorite activities. Our specialists have a variety of tools at their disposal to discover the source of your concerns, determine the best course of action and assess the progress of your treatment.
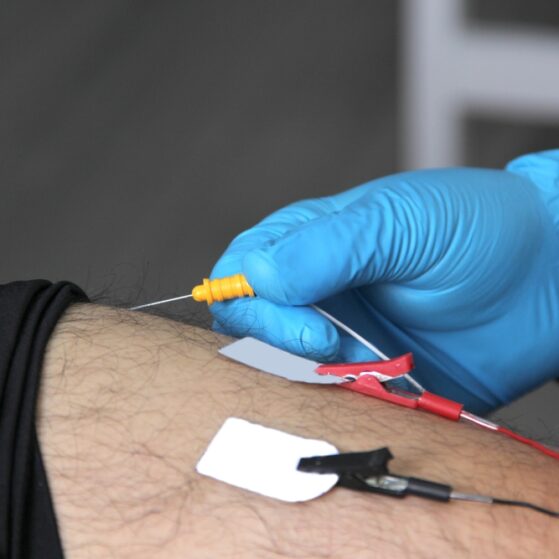
If your provider instructs you to have an electromyography test, or EMG, you may be wondering what exactly this test involves and why you need it. An EMG helps us identify nerve and muscle problems. You can learn more about this type of diagnostic testing below, or reach out to our team with questions.